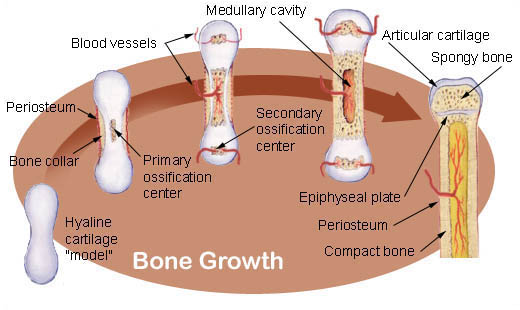
Bone growth and development
The terms osteogenesis and ossification are often used synonymously to indicate the process of bone formation. Parts of the skeleton form during the first few weeks after conception. By the end of the eighth week after conception, the skeletal pattern is formed in the cartilage and connective tissue membranes and ossification begins.
Bone development continues throughout adulthood. Even after reaching adult height, bone development continues for fracture repair and remodelling to accommodate changing lifestyles. Osteoblasts, osteocytes, and osteoclasts are the three cell types involved in bone growth, development, and remodelling. Osteoblasts are bone-forming cells, osteocytes are mature bone cells, and osteoclasts break down and resorb bone.
There are two types of ossification: intramembranous and endochondral.
- Intramembranous
Intramembranous ossification involves the replacement of sheet-shaped connective tissue membranes with bone tissue. Bones formed in this way are called intramembranous bones. They include certain flat bones of the skull and some irregular bones. Future bones first form as membranes of connective tissue. Osteoblasts migrate to the membranes and lay down bone matrix around them. When osteoblasts are surrounded by matrix they are called osteocytes.
- Endochondral ossification
Endochondral ossification involves the replacement of hyaline cartilage by bone tissue. Most of the bones of the skeleton are formed in this way. These bones are called endochondral bones. In this process, future bones are first formed as models of hyaline cartilage. During the third month after conception, the perichondrium surrounding the hyaline cartilage „patterns” becomes infiltrated with blood vessels and osteoblasts and transforms into a periosteum.
Osteoblasts form a collar of compact bone around the diaphysis. At the same time, the cartilage in the centre of the diaphysis begins to disintegrate. Osteoblasts penetrate the cartilage that is breaking down and replace it with cancellous bone. This forms a primary ossification centre. Ossification continues from this centre towards the ends of the bones. After cancellous bone forms in the diaphysis, osteoclasts break down the newly formed bone to open up the marrow cavity.
The cartilage in the epiphyses continues to grow, so the developing bone increases in length. Later, usually after birth, secondary ossification centres form in the epiphyses. Ossification in the epiphyses is similar to that in the diaphysis except that the cancellous bone is retained rather than broken to form a medullary cavity. When secondary ossification is complete, the hyaline cartilage is completely replaced by bone except in two areas. A region of hyaline cartilage remains on the surface of the epiphysis as articular cartilage and another area of cartilage remains between the epiphysis and diaphysis. This is the epiphyseal plate or growth region.
Bone growth
Bones grow in length at the epiphyseal plate by a process similar to endochondral ossification. Cartilage in the region of the epiphyseal plate proximal to the epiphysis continues to grow by mitosis. The chondrocytes, in the region close to the diaphysis, age and degenerate. Osteoblasts move and ossify the matrix to form bone. This process continues throughout childhood and adolescence until cartilage growth slows and eventually stops. When cartilage growth ceases, usually in the early twenties, the epiphyseal plate completely ossifies so that only a thin epiphyseal line remains and the bones can no longer grow in length.
Bone growth is under the influence of growth hormones from the anterior pituitary gland and sex hormones from the ovaries and testes. Although bones stop growing in length in early adulthood, they may continue to increase in thickness or diameter throughout life in response to stress from increased muscle activity or weight. The increase in diameter is called appositional growth. Osteoblasts in the periosteum form compact bone around the outer bone surface. At the same time, osteoclasts in the endosteum break down bone on the inner bone surface around the marrow cavity. These two processes together increase the diameter of the bone and at the same time prevent the bone from becoming excessively heavy and bulky.